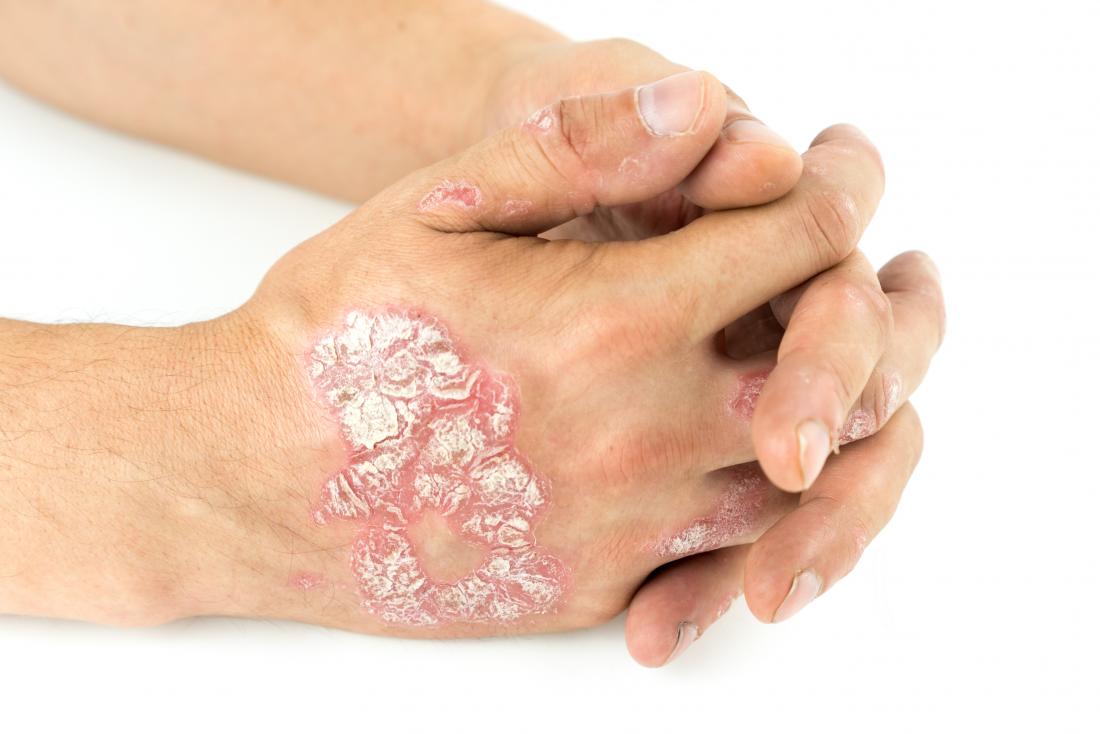
Millions of individuals throughout the world suffer from the chronic skin disorder plaque psoriasis. Although this illness is frequently accompanied by scaly areas of skin, the underlying causes are complicated and yet not fully understood.
Researchers and medical experts have focused a lot on the probable link between autoimmune illnesses and plaque psoriasis, which is an important element of the condition. We’ll get to know about this that “is plaque psoriasis an autoimmune disease” in this blog.
With an emphasis on the function of autoimmune components, we’ll examine the characteristics of plaque psoriasis, its symptoms, causes, kinds, and current therapies. So, let’s continue to learn more:
Understanding Psoriasis
Before we dive into the autoimmune aspects of plaque psoriasis, it’s essential to have a solid grasp of what psoriasis is.
What is Psoriasis?
Skin cells rapidly start accumulating in psoriasis, a persistent skin disorder. Plaques thick, scaly, silvery patches are the outcome, and they frequently itch and are uncomfortable. Psoriasis can affect persons of all ages and is not communicable.
Psoriasis Symptoms
Following are the psoriasis symptoms, which can vary from person to person but often include:
- Red, inflamed skin
- Silvery-white scales
- Itching and burning
- Dry, cracked skin that may bleed
- Thickened or pitted nails
- Joint pain in some cases (known as psoriatic arthritis)
If you see any of these signs or symptoms, then you should consult your healthcare provider.
Psoriasis Causes
While the exact cause of psoriasis is not fully understood, it is believed to be a multifactorial condition. The primary factors include genetics, immune system dysfunction, and environmental triggers. This immune system component is where the autoimmune aspect comes into play.
Is Plaque Psoriasis an Autoimmune Disease?
Significant progress has been made in the knowledge of the autoimmune basis of plaque psoriasis. It is generally acknowledged that the disorder is caused by a malfunction of the immune system when T cells mistakenly target healthy skin cells. How it works is as follows:
Immune Response:
White blood cells, or T cells, aid in defending the body against infection in a healthy immune system. However, the T cells over activate and cause an aberrant immunological response in persons with plaque psoriasis.
Attack on Skin Cells:
The hyperactive T cells attack healthy skin cells rather than warding off infections. This causes an inflammatory reaction, which accelerates the shedding of skin cells and results in the development of plaques.
Cytokines:
These immune response-regulating proteins also contribute to the inflammation in plaque psoriasis. TNF-alpha and IL-17, two distinct cytokines, are critical in the inflammation associated with psoriasis.
Genetic Predisposition:
Since psoriasis frequently runs in families, genetic factors also have an impact. The chance of developing the illness is enhanced by specific genes.
As a result of the immune system attacking healthy skin cells, plaque psoriasis has a strong autoimmune component, even if it is not a traditional autoimmune illness like lupus or rheumatoid arthritis. This causes prominent symptoms.
Psoriasis Types
There are different types of psoriasis, with plaque psoriasis being the most common. Other types include guttate, pustular, inverse, and erythrodermic psoriasis. Each type presents with its unique characteristics and may require specific treatment approaches.
Psoriasis Treatment
Plaque psoriasis treatment frequently consists of a combination of techniques aimed at lowering symptoms, delaying skin cell renewal, and managing inflammation. Options for treatment include:
- Topical treatments include creams, ointments, and shampoos that contain corticosteroids, vitamin D analogs, or coal tar.
- UV light under control can be used in phototherapy to assist in halting the shedding of skin cells.
- Systemic drugs: In extreme situations, oral or intravenous drugs, such as immunosuppressants and biologics, may be recommended.
- Lifestyle modifications: Stress management, eating a balanced diet, and avoiding triggers can all help prevent flare-ups.
A chronic skin disorder known as plaque psoriasis is caused by the immune system mistakenly attacking healthy skin cells. Understanding the immune system’s participation in this condition, even though it may not meet the usual description of an autoimmune disease, is crucial for creating successful treatments.
Consult a healthcare provider if you or someone you know has plaque psoriasis to determine the best course of action and take back control of the condition’s symptoms. Keep in mind that every person with psoriasis is different, so it’s essential to consult a dermatologist to determine the best course of action for you.
How Biologic Infusion Therapy Can Treat Plaque Psoriasis?
In contrast to the majority of traditional psoriasis medications, which target the entire immune system, the most recent infusion medications, or biologics, are more targeted, addressing only the damaged part of the immune system. There are, hence, fewer unanticipated effects and a higher degree of treatment precision.
T-cells from the immune system and other proteins that cause psoriasis are inhibited by psoriasis biologics that are given intravenously or intramuscularly.
Biologics stop some cells or proteins that are involved in psoriasis. They keep them from performing to their greatest potential. That lowers your body’s natural defenses while also reducing inflammation and other issues.
If your immune system is weak, you may be more prone to illnesses or infections. Additionally, it can bring back an illness that your body is already managing, such as tuberculosis (TB).
The biologics for plaque psoriasis include Cimzia, Remicade, Enbrel, Humira, Orencia, Stelara, Consentyx, Skyrizi, etc.
While taking these biological medications, it’s important to keep an eye out for infection signs like fever, chills, and feeling exhausted or achy. In the event that you encounter any of those signs, you ought to see a physician.
Plaque psoriasis injections are utilized to administer these biologics to patients. Consult your doctor to find out if there could be any interactions before starting treatment with any of the aforementioned drugs, especially if you are already on any of them or other biologics.
Fuse Infusion Helps You Overcoming Plaque Psoriasis
If your doctor has recommended biologic infusion therapy treatment for plaque psoriasis, we at Fuse Infusion offer you the best treatment services. We treat plaque psoriasis through plaque psoriasis injections and help our patients in overcoming this chronic disease.
Each Fuse Infusion patient receives direct care and treatment from our licensed professionals throughout biological infusion therapy, providing thorough medical management.
From start to end, each patient receives individualized care. When required, on-call medical professionals are accessible.
At Fuse Infusion, we believe in offering premium-quality services to our patients. So, contact us to receive a biologic infusion today!