Ulcerative Colitis: Symptoms, Treatment, Diet, and Disability Considerations
Ulcerative colitis (UC) is a kind of inflammatory bowel disease (IBD). The severity of the symptoms might range from minor to severe. You may not experience any symptoms in some circumstances. Treatment focuses on symptom management or reduction.
Fuse Infusion offers a biologic infusion therapy treatment and helps you overcome the symptoms of ulcerative colitis in a safe and secure environment.
Understanding Ulcerative Colitis
Ulcerative colitis is an inflammatory bowel disease (IBD) that primarily affects the colon (large intestine) and rectum. It causes chronic inflammation and ulcers in the colon’s inner lining, leading to a range of symptoms. Common symptoms of ulcerative colitis may include:
- Diarrhea: Frequent, loose stools that may contain blood or mucus.
- Abdominal Pain: Cramping and discomfort in the lower abdomen.
- Rectal Bleeding: Blood in the stool or on toilet paper.
- Urgency and Incomplete Bowel Movements: The strong and sudden need to have a bowel movement, often with a feeling of incomplete evacuation.
- Fatigue: Persistent tiredness and lack of energy.
- Weight Loss: Unintentional weight loss due to reduced appetite or malabsorption.
- Loss of Appetite: Reduced interest in eating.
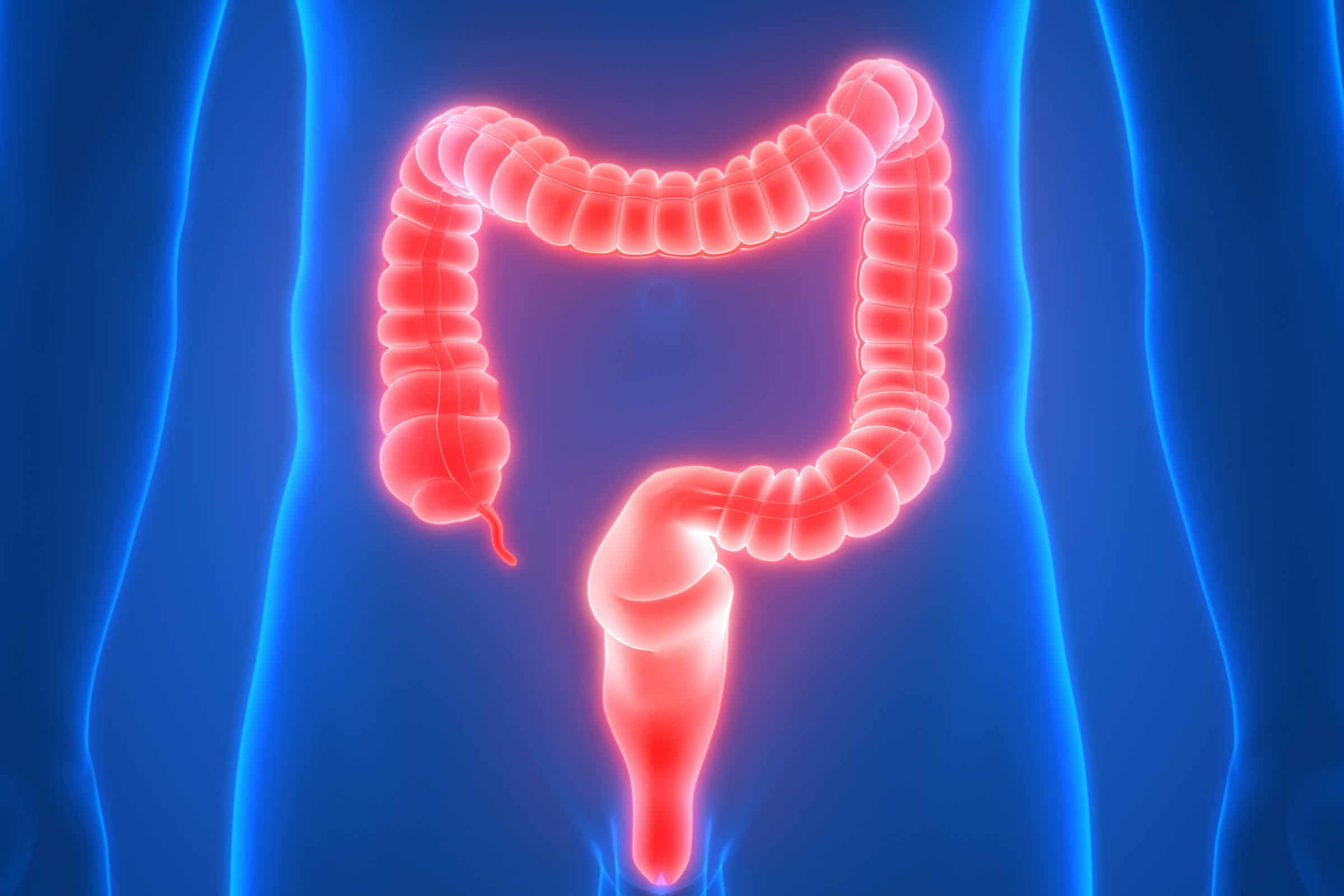
3D Illustration Concept of Large Intestine a Part of Human Digestive System Anatomy X-ray 3D rendering
Ulcerative Colitis Diet
While there is no one-size-fits-all diet for ulcerative colitis, certain dietary considerations may help manage symptoms and promote intestinal health. Here are some general recommendations:
- Low-Residue Diet: Limiting foods that are high in fiber can help reduce bowel movements and ease symptoms. This may involve avoiding seeds, nuts, raw fruits and vegetables, and whole grains.
- Food Diary: Keeping a food diary can help identify trigger foods that worsen symptoms. It’s important to note individual tolerances and make dietary adjustments accordingly.
- Nutritional Supplements: In some cases, nutritional supplements may be recommended to address nutrient deficiencies and support overall health.
- Consultation with a Registered Dietitian: Working with a registered dietitian who specializes in gastrointestinal health can provide personalized dietary guidance and support.
Ulcerative Colitis and Its Impact on Disability
Ulcerative colitis can have a significant impact on an individual’s daily life and functioning. While it is a chronic condition, the impact of disability may vary from person to person. Some factors to consider include:
Fluctuating Symptoms:
Ulcerative colitis is characterized by periods of flare-ups and remission. During flare-ups, symptoms can be severe and significantly impact daily activities, work, and overall quality of life. The unpredictable nature of the disease can make it challenging to maintain regular work attendance and perform tasks consistently.
Treatment Response:
The effectiveness of treatment in managing symptoms and achieving disease control is crucial in assessing the impact on disability. Some individuals may respond well to medication and be able to manage their symptoms effectively, while others may experience more persistent or severe symptoms that affect their ability to work or engage in daily activities.
Functional Limitations:
The physical symptoms of ulcerative colitis, such as frequent bowel movements, abdominal pain, and fatigue, can lead to functional limitations. These limitations may affect an individual’s ability to perform physically demanding tasks, maintain regular work hours, or participate in activities requiring prolonged periods of sitting or standing.
Emotional and Psychological Impact:
The emotional and psychological toll of living with a chronic condition like ulcerative colitis should not be underestimated. The stress, anxiety, and depression associated with the disease can affect an individual’s overall well-being and ability to function optimally in various aspects of life.
Ulcerative Colitis Treatment
Biologic infusion therapy has shown great promise in treating ulcerative colitis, particularly in cases where other treatment options have been ineffective. This therapy involves the administration of biologic drugs, which are derived from living organisms, to target specific components of the immune system that are responsible for inflammation in ulcerative colitis.
Here are some ways in which biologic infusion therapy helps in treating ulcerative colitis:
Targeted Inflammation Reduction:
Biologic drugs used in infusion therapy specifically target certain molecules or cells involved in the inflammatory process of ulcerative colitis. One example is anti-tumor necrosis factor (TNF) drugs, which bind to TNF, a pro-inflammatory protein, and neutralize its effects. By reducing inflammation, these drugs can help alleviate the symptoms of ulcerative colitis and induce remission.
Improved Healing of the Intestinal Lining:
Ulcerative colitis causes ulcers and damage to the lining of the colon. Biologic infusion therapy can promote the healing of these ulcers by modulating the immune response and reducing inflammation. This can help restore the integrity of the intestinal lining and improve overall gut health.
Maintenance of Remission:
Biologic infusion therapy has been effective in maintaining remission in individuals with moderate to severe ulcerative colitis. By suppressing the immune system’s inflammatory response, these drugs can help prevent flare-ups and prolong periods of remission. This is especially beneficial for individuals who have had recurrent episodes of active disease despite other treatment approaches.
Reduction in Steroid Dependence:
Steroids, such as prednisone, are commonly used to manage acute flare-ups of ulcerative colitis. However, long-term use of steroids can have significant side effects. Biologic infusion therapy can help reduce the need for prolonged steroid use by providing a targeted and effective treatment option to replace or reduce reliance on steroids.
Individualized Treatment Approach:
Biologic infusion therapy is tailored to the individual’s specific disease characteristics and response to other treatments. Healthcare providers can assess the patient’s condition and determine the most appropriate biologic drug based on factors such as disease severity, previous treatment history, and genetic markers. This personalized approach helps optimize treatment outcomes and minimize potential side effects.
It’s important to note that biologic infusion therapy is typically used for individuals with moderate to severe ulcerative colitis who have not responded well to conventional treatments, such as aminosalicylates, corticosteroids, or immunomodulators. The therapy is administered in specialized healthcare settings under the supervision of trained medical professionals.
As with any medical treatment, biologic infusion therapy may have potential risks and side effects. It is essential to discuss the benefits and potential risks with your healthcare provider to make an informed decision regarding the suitability of this therapy for your specific condition.
Contact Fuse Infusion for Ulcerative Colitis Treatment
If your doctor has recommended biological therapy treatment for ulcerative colitis, we at Fuse Infusion offer you the best treatment services. We treat ulcerative colitis through medications, which are specialized biologics, and help our patients in overcoming this chronic disease.
Each Fuse Infusion patient receives direct care and treatment from our licensed professionals throughout biological infusion therapy, providing thorough medical management.
From start to end, each patient receives individualized care. When required, on-call medical professionals are accessible.
At Fuse Infusion, we believe in offering premium-quality services to our patients. So, contact us to receive a biological infusion today!